In 2007, Japan reached the level defined by the World Health Organization as a “super-aged society”—i.e., 21 percent or more of the population is aged 65 and older—and since then, its elderly population has continued to grow. In particular, the number of those who are “old-old” (80 years old and up) has markedly increased, rising above 10 million for the first time in 2015. As a result, the scarcity of care workers has become a major concern in Japan, and it is predicted that in 2025, the shortfall in the number of caregivers will reach 370,000 workers.
As people reach the age of 80 and higher, there is an evident increase in frailty and debility. As an elderly person becomes increasingly frail, they face an increasing number of daily tasks that they are no longer able to carry out on their own, and without the support of a care worker, they would become confined to their bed. In order for seniors to avoid that fate and be able to continue with their daily routines, care workers play a critical role. But depending on how that caregiver provides that assistance, it has been noted that the task of caregiving can actually have a negative impact on their own health.
Up until now in Japan, caregiving in practice has relied on the caregiver’s individual strength when assisting the care recipient, although the methods vary from person to person. In particular, transfers—moving seniors from a wheelchair to a bed or to a toilet, for example—often require the caregiver to lift the person. But that process often places excessive strain on the caregiver’s body, leading to back injuries. It has been reported that roughly 60 percent of nurses and caregivers in Japan suffer from back pain, and many are forced to leave the profession as a result. Manually transferring a person can have a negative impact on the care recipient as well. Falls, abrasions, skin tears, and other injuries can occur as caregivers lift and pull their elderly care recipients. Such injuries can make seniors apprehensive about receiving care. Also, because the manual transfer process often means that the senior receiving care must relax and yield to the force being exerted by the caregiver, it reduces the opportunity for them to use their own physical capabilities, thereby encouraging the development of disuse syndrome.
In order to improve this situation, the No Lifting Association (NLA) has worked with Professor Hajime Asama of Tokyo University to develop and popularize a system of “no-lift care,” a scientifically based system that allows caregivers to care for the elderly without relying solely on the caregiver’s physical strength. The NLA spoke with Japanese care workers about their experiences and clarified the type of information that caregivers convey to their patients. The researchers also analyzed the movements care workers undertake in their work in order to create a visualization of what they do. In addition to this scientific data, they examined the No Lifting Policy Training Program offered by the Australian Nursing Federation, which allowed them to create a Japanese version of a caregiver training program that will help them popularize no-lift care.
The no-lift care concept focuses on three points: (1) caregivers should not limit elderly care recipients’ opportunities to move on their own (i.e., let them do what they can do on their own), (2) caregivers should be prohibited from relying entirely on their strength to “push, pull, lift, twist, and carry,” (3) the appropriate assistive technologies should be used.
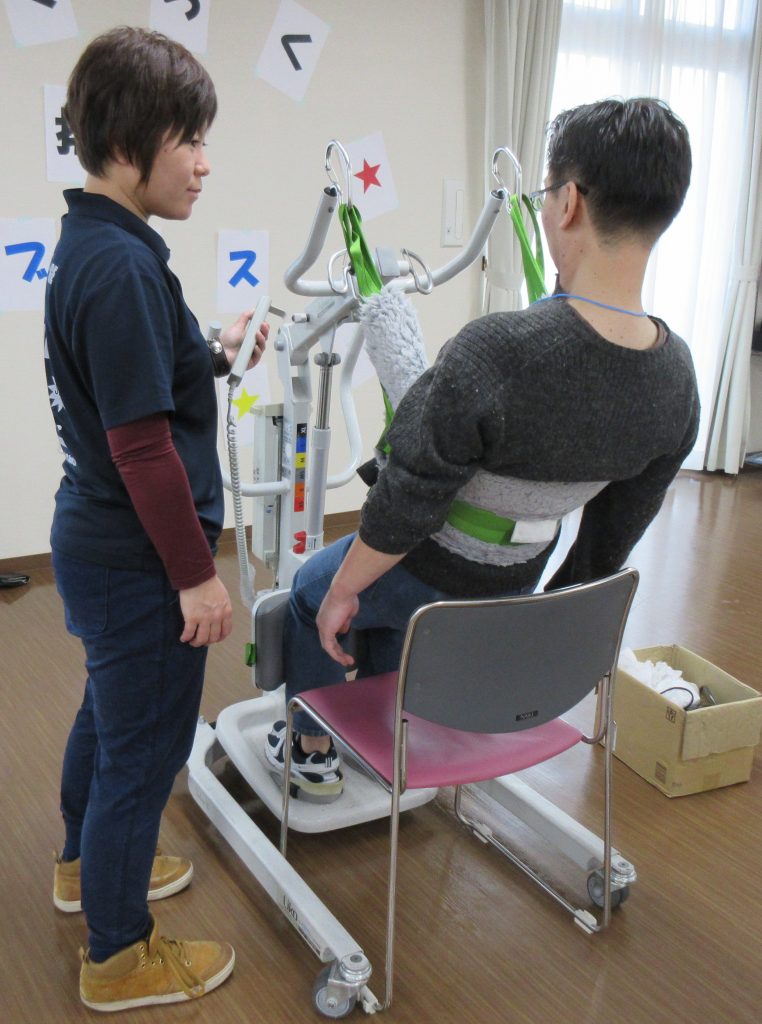
For example, let us look at the case of transferring a senior from a bed to a wheelchair. In the past, caregivers relied on their own physical strength, and so in order to prevent the elderly care recipient from falling between the bed and the wheelchair, the caregiver would lift the person’s bottom and transfer them into the wheelchair. With the no-lift care concept, a standing machine supports a senior standing from the bed so that the caregiver does not have to exert as much effort and the senior care recipient can transfer to the wheelchair using their own physical capabilities (see photo). In other words, the no-lift care concept that “caregivers should not help care recipients with things they can do themselves” helps seniors maintain their ability to carry out daily activities while receiving the care they need.
Junko Yasuda, president of the NLA, wants to make sure that “no-lift care” becomes widely understood and adopted. In order to encourage that, the NLA has been carrying out coordinator training programs since 2015, and there are currently 141 trained “no-lift care coordinators” working throughout Japan.As countries throughout Asia face the aging of their societies as well, this concept of providing smarter care that does not rely solely on the strength of the caregiver can offer an important hint to improve the health outcomes for caregiver and care recipient alike.

Related Resources
No Lifting Association website (Japanese)

