2020 HAPI Grand Prize Winner
As populations age, it will be of key importance to develop systems that empower people to maintain their self-reliance and independence as they grow older. In Komagane City, Nagano Prefecture, Japan, the local government has partnered with Showa Inan General Hospital to do just that through a patient-centric program that focuses on preventing stroke recurrence among older people after they have been discharged from hospital. In collaboration with the hospital, Komagane City has created a path of support for stroke patients that begins with hospitalization and continues for one year following their discharge.
As Komagane City looked at options to create a healthier and age-friendly city, they realized that strokes were a major issue for their residents as a life-threatening and life-altering disease. Working with the local hospital, they identified that cerebral disease was the most common form of illness amongst older people transported to hospital via ambulance. In addition, they discovered that the stroke recurrence rate was highest in the first year after discharge, with 60 percent of recurrences occurring in those with mild symptoms who could still walk. But simply providing information and encouraging discharged patients to change their diet and lifestyles would not solve the problem.
Komagane City and Show Inan General Hospital Acceptance Video
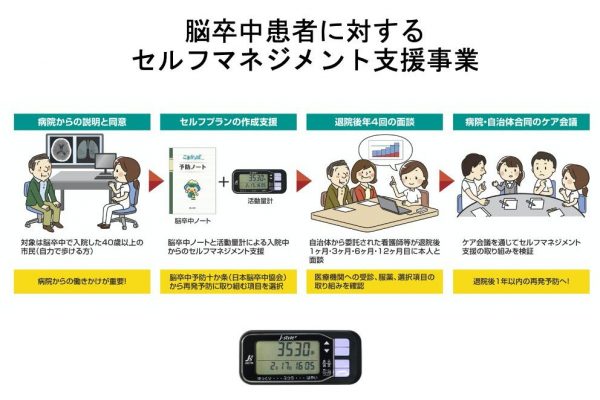
As a result, they developed a program through which skilled professionals work to educate patients and their families during the patient’s hospitalization. They create a care plan, teach the patient how to monitor their vital signs, and have them record them using a “prevention notebook,” in which patients set their own goals. Involving the patient in this process of self-planning and self-monitoring encourages them to be aware of their disease and health status so that they can adopt a healthier lifestyle and improve their “self-management capability.”
The path of support continues once the patient is discharged as the registered nurse in charge will share information with the patient’s personal physician and will hold consultations with them and their families four times over the course of the year (1, 3, 6, and 12 months after discharge) to ensure that patients are sticking to their plan to achieve their initial goals.
This process is supported through a special “My Page” website developed by the local government, which allows patients to monitor their daily condition and explain that to their personal physician. The page can be viewed from a smartphone and can wirelessly record daily activities such as the number of steps taken, as well as be used to record vital data (blood pressure, weight, temperature, etc.).
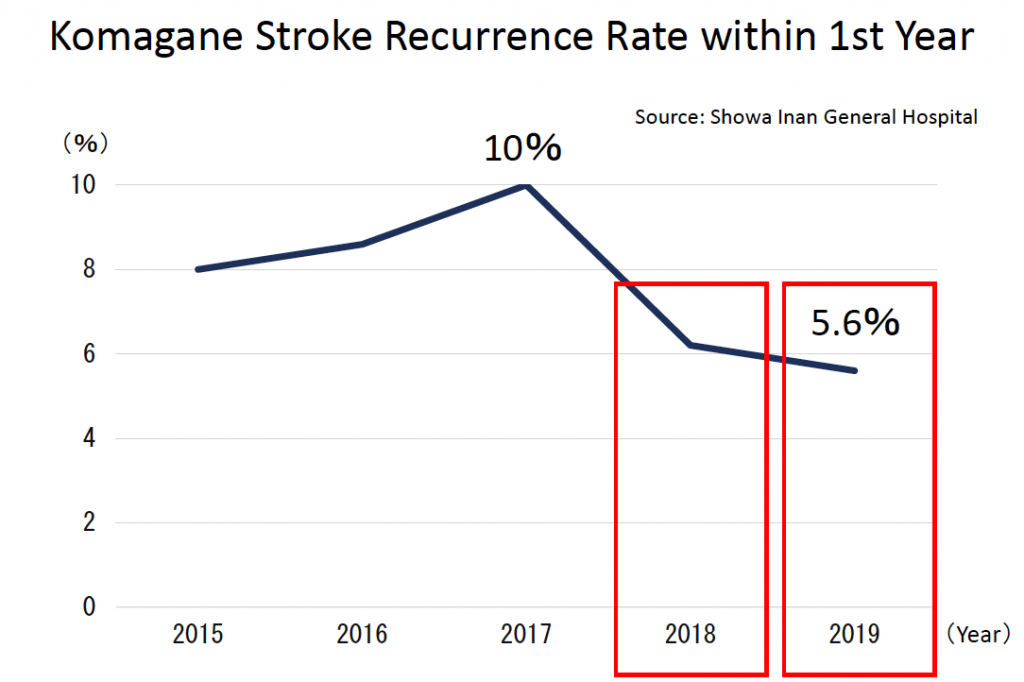
By intentionally targeting patients with mild strokes, they were able to see significant improvements in outcomes for stroke patients. Before starting the program, the stroke recurrence rate was over 8 percent, but after implementing the project in FY2018 it dropped to 6.2 percent and has fallen further still to 4.8 percent in FY2019. This success has meant they are considering extending the scope of the program to target other chronic illnesses such as cardiac issues in the future.
A two-year pilot program implemented before rolling out the whole program also played a key role in the success of the program. The pilot allowed them to build consensus and create common understanding between partners and stakeholders including the local government, medical facility, and care facility personnel. It also allowed them to properly incorporate and improve the patient education and self-management aspects of the program. As one example, they started having patients take their own blood pressure while still in hospital so that they would be comfortable doing so once they returned to home after discharge.
KEYS TO SUCCESS
- The patient-centric approach and use of the city’s “My Page” website encouraged patients to take charge of their own health management
- The close relationship between the hospital and local government allowed for the creation of a path of support after hospital discharge
- The two-year pilot program built consensus and common understanding between partners and allowed for improvements in patient education
- Data was used to select the right target group and ensure that the intervention had the most significant impact